Satoshi Hirahara, a doctor at Kajiwara Clinic, checks protective clothing to be used for home visits in Kita Ward, Tokyo, on Feb. 15.
9:40 JST, February 28, 2021
Medical care for COVID-19 patients recuperating at home has emerged as an important issue amid the third wave of the novel coronavirus.
Satoshi Hirahara, a doctor at Kajiwara Clinic in Kita Ward, Tokyo, was stunned when he was told, “We can’t find a place for the patient to be hospitalized,” during a phone call with a public health center in mid-January.
Hirahara had made a house call and conducted an antigen test on a male patient in his 90s, who lived alone and had been suffering from fever since early January.
The antigen test came back negative and he was admitted to a nearby hospital with suspected pneumonia. However, the patient was sent back home when a PCR test showed a positive COVID-19 result. The hospital did not have beds for COVID-19 patients and another hospital could not be found to accept him.
With mild dementia, pneumonia symptoms and a fever running from 37 to 38 C, Kajiwara Clinic hurriedly set up a special system to keep watch over him.
Hirahara began visiting the patient’s house every evening. To avoid outing himself as a doctor making house calls during a pandemic, he put on his protective clothing and goggles after entering the home. He then checked the patient’s temperature, blood oxygen level, facial color, breathing and also administered medication.
Fortunately, the man’s condition did not worsen and his symptoms subsided. “If an elderly person with a high risk of serious illness has to be treated at home, it is not enough for the public health center to [only] monitor a patient’s health by phone,” Hirahara said.
Easing the burden
Checking on patients at their homes has typically come under the purview of public health centers. But with the pandemic upping the pressure, dealing with every patient — including those with mild symptoms — could potentially exceed centers’ capabilities. To ease the burden, an increasing number of clinic doctors have begun to monitor patients recuperating at home.
In Shinjuku Ward, Tokyo, doctors engaged in home medical care offer telephone consultations. This effort was started by Shinjuku Hiro Clinic doctor Hiroo Hanabusa on a voluntary basis last summer. Since December of last year, he has been taking turns with other clinics as part of a project commissioned by the ward government.
The doctors have received comments from patients with mild symptoms such as, “Can I take an antipyretic?” or, “I have eczema.” They also make house calls as needed.
During one such visit, a female patient in her 70s was mildly ill with a fever of 37 C, but a blood test showed an inflammatory reaction. After that, the progress of her symptoms was checked daily by phone.
During a house call three days later, her blood oxygen level had dropped significantly, so she was hospitalized for treatment.
“It is essential to check the health of patients who are recovering at home or in hotels,” Hanabusa said.
Health centers stretched
During the third wave, the nation has faced a growing shortage of hospital beds to treat COVID-19 patients, which has led to many recuperating at home.
According to the Health, Labor and Welfare Ministry, 35,394 people nationwide were recuperating at home as of Jan. 20. In Tokyo, the number of people infected with the disease who were not yet assigned to a medical institution exceeded 7,000 in mid-January.
Under normal circumstances, it is the job of public health centers to monitor the health of patients recuperating at home.
Public health nurses and other staff usually pick up the phone and call patients to ask them about their condition. However, the pressure on the medical system has reached a level where staff have been too swamped to adequately monitor their patients, because they have to deal with newly infected people and investigate infection routes.
Since April last year, the ministry has requested that local governments, medical associations and medical institutions cooperate with each other, saying that medical knowledge is also necessary to monitor the health of people recuperating at home. Yet such cooperation has yet to prove fruitful.
Many doctors have been hesitant about monitoring such patients at home, with some saying, “We are not sure if we can implement sufficient infection control measures,” or “Who will take responsibility if a patient dies at home?” according to sources close to a medical association.
Online services also option
Meanwhile, the Chofu Medical Association in Tokyo has drawn attention for its progressive efforts in taking care of patients recuperating at home. Nine clinics in the Chofu area were cooperating as of Feb. 15 to provide round-the-clock telephone consultations and house calls to such patients.
The clinics are supposed to telephone patients at high risk of becoming seriously ill after receiving requests from the public health center. House calls are made if deemed necessary.
The city subsidizes ¥30,000 per home visit and ¥10,000 per phone consultation.
They are also considering the use of online medical services.
“We want to create a system where the entire community can look after patients,” said Shinichi Nishida, chairman of the Chofu Medical Association.
“Even if there are no obvious symptoms, the novel coronavirus can cause pneumonia and other diseases. In many cases, it is necessary for a doctor to do an examination to promptly notice changes in [a patient’s] condition,” Tetsuya Matsumoto, a professor at the International University of Health and Welfare, said. “It is a heavy burden for doctors to make house calls all the time, which is why we need to consider efficient systems such as online medical services.”
Top Articles in Society
-
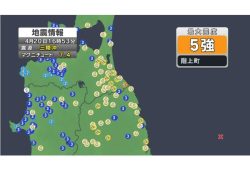
Earthquake Hits Japan’s Tohoku Region; 3-meter Tsunami Warning Issued (Update 1)
-

Police Find Child’s Shoe During Search for Missing Boy in Nantan, Kyoto Prefecture
-

Body Found in Nantan, Kyoto Prefecture, During Search for 11-Year-Old Boy in Area (Update 1)
-

Cherry Blossoms, Rapeseed Flowers Perform Colorful ‘Duet’ in Niigata
-

Japan to Ban Use of Portable Chargers on Airplanes from April 24, Number of Regular Chargers To Be Limited to 2
JN ACCESS RANKING
-

Earthquake Hits Japan’s Tohoku Region; 3-meter Tsunami Warning Issued (Update 1)
-

Police Find Child’s Shoe During Search for Missing Boy in Nantan, Kyoto Prefecture
-

Body Found in Nantan, Kyoto Prefecture, During Search for 11-Year-Old Boy in Area (Update 1)
-

Cherry Blossoms, Rapeseed Flowers Perform Colorful ‘Duet’ in Niigata
-

China, South Korea Object to Japanese PM Takaichi’s Ritual Offering to Yasukuni Shrine
Most read in the last 24 hours
-

India’s Arms Indigenization Quest for Self-Reliance / Big Firms, ...
-

Japan Moves Closer to Blocking Illegal Online Casinos as Governme...
-

Shifts Startup Focus to Nurturing Global Winners
-

Princess Aiko Enjoys Imperial Court Music, Dance; Production, Cos...
-

Bibimbap with Spring Vegetables and Asari Clam Miso a Rich Taste ...
Most read in the last 7 days
-

Earthquake Hits Japan's Tohoku Region; 3-meter Tsunami Warning Is...
-

China, South Korea Object to Japanese PM Takaichi's Ritual Offeri...
-

Trump Extends the Ceasefire with Iran but Keeps the Blockade
-

India's Arms Indigenization Quest for Self-Reliance / New Delhi S...
-

¥1,000 Coins to Be Issued to Mark Anniversary of Beginning of Jap...
Most read in the last 30 days
-

Earthquake Hits Japan's Tohoku Region; 3-meter Tsunami Warning Is...
-

Police Find Child's Shoe During Search for Missing Boy in Nantan,...
-

Body Found in Nantan, Kyoto Prefecture, During Search for 11-Year...
-

Cherry Blossoms, Rapeseed Flowers Perform Colorful ‘Duet’ in Niig...
-

China, South Korea Object to Japanese PM Takaichi's Ritual Offeri...